- Contents
In October 2021, as much of the world focused on the distribution of COVID-19 vaccines, the World Health Organization (WHO) made a historic recommendation for widespread use of the malaria vaccine among at-risk children under the age of five. The recommendation is based on the results of an ongoing pilot program that began in 2019 in the high-transmission countries of Ghana, Kenya, and Malawi. The program involved more than 800,000 children.
An effective malaria vaccine has the potential to change the face of children’s health in high-burden countries. More than 260,000 African children succumb to malaria each year. “This is a historic moment. The long-awaited malaria vaccine for children is a breakthrough for science, child health, and malaria control,” said WHO Director General Dr Tedros Adhanom Ghebreyesus. “Using this vaccine on top of existing tools to prevent malaria could save tens of thousands of young lives each year.”
GAVI, the Vaccine Alliance, announced its intentions in December 2021 to help fund the rollout of the vaccine in sub-Saharan Africa. Others in the global health community, including GlaxoSmithKline (GSK), PATH, and UNICEF, have also stepped in to boost production of the vaccine.
Vaccine production is only one part of the equation, however. Demand is also crucial. As witnessed in the current COVID-19 crisis, vaccine demand often hinges on public perception. With childhood vaccines, including the new malaria vaccine, the perceptions of parents are the most consequential.

To explore parents’ perceptions of the new and potentially revolutionary malaria vaccine, GeoPoll conducted an SMS mobile phone-based survey in February 2022 in several high-burden malaria countries: three from the original vaccine trial (Ghana, Kenya, and Malawi), as well as Nigeria, the Democratic Republic of the Congo (DRC), Uganda, and Mozambique. The survey addressed a number of topics related to the vaccine, including:
- Parent perceptions of routine childhood vaccines
- Awareness of the new malaria vaccine
- Intent to vaccinate for malaria and reasons for hesitancy
- Impact of COVID-19 vaccines on parent perceptions
Findings from the survey are summarized in this post. To view the full results, filterable by question, country, gender, and age group, scroll down to the Interactive Data Dashboard.
As part of this study, additional data was collected using questions grounded in Social and Behavior Change (SBC) theory. GeoPoll considered it crucial to ground certain survey questions in SBC theory to help inform communication interventions going forward. The findings from that component of the study will be released in the coming months.
Methodology
The study questionnaire was designed by GeoPoll researchers in collaboration with PATH. PATH, the nonprofit global health organization, has been involved in the development and introduction of this malaria vaccine since 2001.
The study was conducted in English in Ghana, Kenya, Malawi, Nigeria, and Uganda; French in the Democratic Republic of Congo; and Portuguese in Mozambique (7 countries total).
The sample size for the study was 400 respondents per country and 2,800 total. Although not purely scientific as there were no strict measures to limit demographic quotas, a diverse mix was achieved, with a gender composition of 43% females and 57% males; an age breakdown of 26% ages 18-25, 37% ages 26-35, and 36% ages 36 and over; and representation from every ADM1 location within each country.
All respondents were parents, with at least 1 child ages 5 or younger living at home.
It is important to note that this study is just an assessment of a relatively small sample of parents’ perceptions about the new malaria vaccine. The goal of this study is to draw attention to the topic and promote further larger-scale scientific research needed to direct complex public health policies.
Routine Childhood Vaccinations
Over the past few decades, the expansion of childhood vaccination services has helped prevent the deaths of millions of children each year. Yet despite tremendous progress, many children around the world have insufficient access to vaccines – particularly in low- and middle-income countries, including many countries in sub-Saharan Africa.
Vaccine coverage rates vary significantly between and within countries, however. In our study, the percentage of parents that have or intend to vaccinate their youngest child (routine childhood vaccinations) ranges from 76% in Malawi to 95% in Uganda. The percentages remain consistent regardless of the age or gender of the parent.
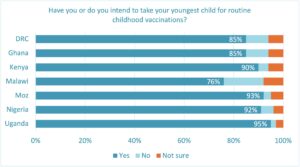
Although the fact that 88% of parents overall have or intend to vaccinate their youngest child illustrates the progress of recent years, that percentage still lags behind other regions of the world according to WHO.
At least part of the reason for that lag can be attributed to the perceived benefit of vaccines. Although more than 30 million African children under the age of five suffer from vaccine-preventable diseases every year, and half a million die, only 81% of parents in our study “strongly agree” with the statement that vaccines benefit their child’s health. That number drops down to 75% in Malawi and 67% in Ghana. Parents in Mozambique are the most likely to strongly agree with the statement at 91%.
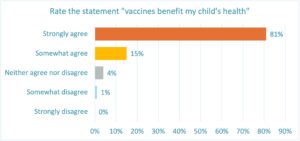
While only 1% of respondents overall disagree that vaccines benefit their child’s health, the fact that 15% “somewhat agree” shows at least some level of vaccine hesitancy.
Malaria Vaccine Awareness and Intent
WHO helped launch the malaria vaccine pilot program for children in Ghana, Kenya and Malawi in 2019. The success of the program led to the organization’s recommendation for widespread use of the vaccine in endemic countries in October 2021.
As Ministries of Health and international partners work to accelerate production, procurement, and deployment of the malaria vaccine, we asked parents in sub-Saharan Africa several questions to assess their awareness of and demand for the new vaccine.
Overall, less than half of the parents surveyed (44%) say they have heard of the new malaria vaccine.
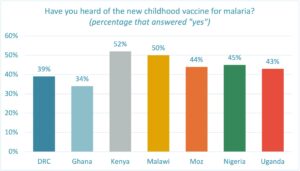
Although the pilot program appears to have heightened awareness in Kenya (52%) and Malawi (50%), parents in Ghana are least likely to have heard of the vaccine at 34%. None of the non-pilot countries top 45% in awareness.
Across sub-Saharan Africa, the opportunity and need clearly exist for governments and global health partners to promote the vaccine as it becomes available.
Despite relatively low awareness of the new vaccine at this stage, demand is fairly high. Overall, 81% of parents in our study say they intend to take their child to get the malaria vaccine if it is available. The percentages range from 76% in Ghana and Malawi to 88% in Mozambique.
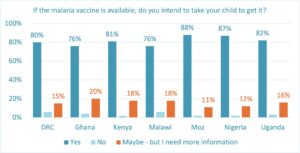
Convenience does not appear to be an obstacle. Across countries, 93% of parents say they would make an extra visit to a health center to get their child immunized if required.
Only 3% of respondents say they do not intend to take their child to get the malaria vaccine and would not make an extra visit to do it if required. Their justification is distributed between, “my children are protected from malaria already” (36%), “I don’t know enough about the vaccine” (36%), and “my children get enough vaccines already” (27%).
The 15% of parents who say they might get their child vaccinated but need more information is understandable considering most were unaware of the vaccine prior to the survey. The information they are most interested in is whether the vaccine is safe (58%), followed by if it will help if they already have bed nets (26%).
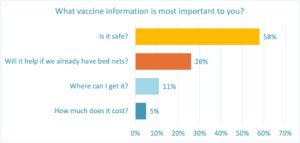
Providing parents with information about the malaria vaccine’s safety and effectiveness should be a priority for governments and other stakeholders.
Impact of the COVID-19 Vaccines
The ongoing COVID-19 pandemic has pushed vaccines to center stage. The race to develop and rollout vaccines in the fight against COVID-19 is a testament to modern science. From the beginning, however, false information and myths about the vaccines spread almost as quickly as the virus, leading to political strife, conspiracy theories, and vaccine hesitancy.
In this environment of heightened vaccine awareness and sensitivity, we asked parents if the COVID-19 vaccine changed their perceptions about vaccines.
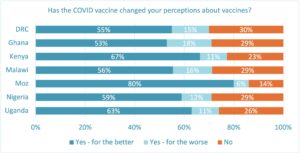
Most respondents across countries (62%) say the COVID-19 vaccine did change their perceptions about vaccines – for the better. That viewpoint is especially prevalent in Mozambique (80%). Mozambique recently reported its first day of zero COVID-19 infections since the pandemic began, and authorities largely attribute the milestone to the country’s mass vaccination campaign.
No higher than 18% of respondents in any country say the COVID-19 vaccine changed their perceptions about vaccines for the worse.
More than half of respondents (51%) have gotten their information about the COVID-19 vaccines from “Radio and TV,” emphasizing the importance of that medium for pushing out information about the new malaria vaccine. The next most relied upon information source is “healthcare workers” at 24%.
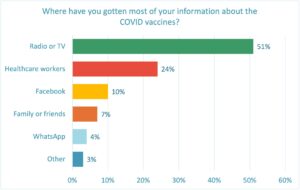
The sources used remain relatively consistent across countries, gender and age group.
Conclusion
Malaria remains a primary cause of childhood illness and death in sub-Saharan Africa. The region carries a disproportionately high share of the global malaria burden, with children’s risk of both contracting and dying from the illness far higher than anywhere else in the world.
WHO’s historic recommendation for the widespread use of the new malaria vaccine in October 2021 reignites hope for the eventual eradication of malaria on the continent. Although less than half of parents in our study had heard about the new malaria vaccine prior to the survey, demand is high, with 81% saying they intend to take their child to get the malaria vaccine if it is available. Understandably, some parents are hesitant until they get more information – particularly about whether the vaccine is safe.
Most parents in our study believe that vaccines benefit their children’s health, and the COVID-19 vaccines have only strengthened that perception. If governments and the global health community continue their efforts to boost production, deployment, and awareness of the new malaria vaccine, the opportunity exists to take significant steps forward in the decades-long battle against the deadly disease.
Interactive Data Dashboard
Dive deeper into the full results from this study using the interactive dashboard below. The dashboard provides responses to each question in the survey, filterable by country, age group, and gender.
Collecting Data for International Development and Relief
This study was implemented by GeoPoll via SMS using our own mobile research platform and respondent database. Data collection occurred from January 28 to February 23, 2022, with some countries completing data collection earlier than others.
GeoPoll has developed unique remote research systems, a large respondent database, and the experience to be able to assist essential humanitarian interventions through the provision of fast, reliable information in any circumstance.
We have worked with international development groups and governments on myriad topics, including humanitarian aid, education, employment, food security, combatting violent extremism, climate change, disease outbreaks, and financial inclusion, among many others. For more information about GeoPoll’s capabilities conducting humanitarian research around the world, please contact us.
